Disc Herniations Explained
- Taylor Austin
- Feb 7
- 5 min read
Chiropractic guidance for acute disc herniation pain, sciatica, and flare-up recovery
If you’ve ever experienced an acute disc herniation flare-up, sciatic pain, or sudden low back or neck pain, you know how intense and overwhelming it can feel. Sudden pain, difficulty moving, nerve symptoms, and fear about making things worse are all very real parts of the experience.
The good news? Most acute disc flare-ups improve with the right support, patience, and a plan that respects how the nervous system and tissues heal. This guide will help you understand what’s happening during an acute disc flare, what to focus on in the early phase, and simple steps you can take to help your body settle and recover.
What Is an Acute Disc Herniation?
(Understanding disc herniation pain, nerve irritation, and flare-ups)
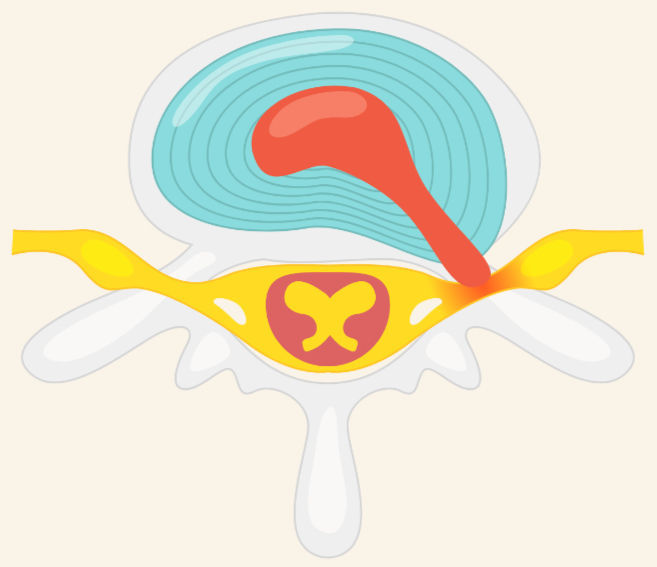
Your spinal discs sit between the vertebrae and act as shock absorbers. A disc herniation occurs when the inner material of the disc pushes outward, sometimes irritating nearby nerves.

An acute flare-up refers to a sudden increase in disc-related symptoms, which may include:
Sharp or deep back or neck pain
Pain radiating into the arm or leg
Tingling, numbness, or burning sensations
Muscle guarding or spasms
Difficulty standing upright or changing positions
Importantly, pain intensity does not always equal the severity of the injury. Acute pain often reflects irritation and nervous system sensitivity, not damage that is actively worsening.
The First Priority: Calm the System
During an acute flare-up, your body’s protective systems are on high alert. Muscles tighten, movement feels threatening, and even small actions can feel overwhelming.
Early on, the goal is not to “fix” the disc, but to:
Reduce irritation
Create a sense of safety for the nervous system
Maintain gentle movement without provoking symptoms
This phase is about settling, not pushing.
What to Do in the First Few Days After a Disc Herniation Flare-Up
1. Respect Pain, But Don’t Freeze Completely
Complete bed rest is rarely helpful, but aggressive stretching or pushing through pain can prolong recovery.
Aim for:
Short, frequent bouts of comfortable movement
Changing positions often (sitting, standing, lying)
Avoiding prolonged positions that increase symptoms
If a movement increases pain significantly or causes symptoms to travel further down the arm or leg, it’s a sign to back off.
2. Use Breath to Reduce Guarding
Pain often creates shallow, upper-chest breathing, which increases muscle tension and nervous system activation.
Gentle diaphragmatic breathing can help:
Reduce protective muscle tone
Improve circulation
Signal safety to the nervous system
Even 2–3 minutes at a time can make a difference.
3. Choose Positions That Reduce Symptoms
Everyone’s disc flare-up behaves a little differently. Some people feel relief lying on their back, others on their side, and some feel better standing.
Common supportive options include:
Lying on your back with knees supported
Side-lying with a pillow between the knees
Short walks if standing feels better than sitting
Pay attention to which positions reduce symptoms rather than chasing a “perfect” posture.
Gentle Movement That Often Helps During an Acute Disc Herniation
These movements are meant to be pain-free or pain-reducing, not intense stretches.
1. Supported Breathing on Your Back

Lie on your back with knees bent or supported
One hand on your ribs, one on your belly
Slowly inhale, feeling the ribs expand
Long, relaxed exhale
Start with 5–8 slow breaths
2. Pelvic Tilts (Small Range)

Lying on your back, gently rock the pelvis
Move only through a comfortable range
Focus on smooth, slow motion
5–10 gentle repetitions
3. Marches into Deadbugs (level 1-3)


Start on your back and lift one foot at a time
Keep your pelvis and ribs steady
Progress to a dead bug variation if you can move without strain
Focus on control and steady breathing
5–10 gentle repetitions alternating each side
4. Hip Bridges

Press through your feet to gently lift your hips
Stop where you feel stable
Engage your glutes and keep your ribs relaxed
Breath easy
Progress levels only if the movement feels smooth and supported
5. Prone Breathing / Sphinx

Lie on your stomach (add pillow under your hips if for comfort)
Breathe into the back and sides of your ribs, keeping your neck and shoulders relaxed
If comfortable, come onto your forearms into sphinx for a gentle stretch
What to Avoid During an Acute Flare-Up
In the early phase, it’s usually best to avoid:
Aggressive stretching into pain
Heavy lifting or twisting
Long periods of sitting
Trying to “push through” nerve symptoms
Healing is not linear, and flare-ups do not mean failure.
When to Seek Professional Support for Disc Herniation Pain
While many disc flare-ups improve with conservative care, you should emergency care if you experience:
Progressive weakness
Loss of bladder or bowel control
Numbness in the saddle region
Pain that continues to worsen despite rest and modification
How a chiropractor can help:
Assessing movement and nerve irritation
Supporting spinal and joint mobility safely
Guiding you through phase-appropriate movement
Helping you return to activity with confidence
The Bigger Picture: Discs Heal Better Than You Think
Discs are living tissues with the ability to adapt and recover. Many people with disc herniations return to full, active lives without surgery.
The key is:
Respecting the acute phase
Gradually restoring movement
Supporting the nervous system
Having guidance when needed
If you’re currently dealing with a disc herniation flare-up, sciatica, or acute back pain and want support navigating recovery, you don’t have to do it alone.
If you’re looking for chiropractic care for disc herniation or sciatica in Burnaby, an individualized assessment can help guide safe movement, reduce irritation, and support long-term recovery.
Frequently Asked Questions About Acute Disc Herniation Flare-Ups
How long does an acute disc herniation flare-up last?
Most acute disc herniation flare-ups improve over a few days to several weeks, depending on the level of irritation, your activity levels, and how well the nervous system is able to calm. Pain often settles before the disc itself has fully healed. A flare-up does not mean permanent damage or that healing has stopped.
Should I rest or keep moving after a disc herniation flare-up?
Relative rest is helpful, but complete bed rest is usually not recommended. Gentle, pain-free movement helps maintain circulation, reduce stiffness, and signal safety to the nervous system. The goal is to move within tolerance, avoiding movements that significantly worsen pain or cause symptoms to travel further down the arm or leg.
Is walking good for a disc herniation?
Yes, short and comfortable walks are often one of the best early activities for disc herniation flare-ups. Walking encourages gentle spinal motion and nervous system regulation. Keep walks short, stop before symptoms increase, and build up gradually.
Should I stretch my back if I have a disc herniation?
In the acute phase, aggressive stretching can sometimes increase irritation. Instead of forcing stretches, focus on gentle movements and breathing that reduce symptoms. As pain settles, targeted stretching and strengthening can be safely reintroduced with guidance.
Can a disc herniation heal on its own?
In many cases, yes. Discs have the ability to adapt and heal over time, and many people recover without surgery. Supportive care, gradual movement, and nervous system regulation play an important role in recovery.
When should I worry about disc herniation symptoms?
You should seek immediate medical attention if you experience:
Progressive or sudden weakness
Loss of bowel or bladder control
Numbness in the groin or saddle region
These symptoms are rare but require urgent assessment.
Can chiropractic care help with disc herniation pain?
Chiropractic care can help many people with disc herniation or sciatica by improving joint mobility, reducing muscle guarding, and supporting nervous system regulation. Care should always be individualized and appropriate for the acute phase, focusing on comfort, safety, and gradual return to movement.
This blog is for educational purposes and does not replace individualized medical care. If you’re unsure what movements are appropriate for you, seek professional guidance.




Comments